What is depression and how does it affect veterans?
Major Depressive Disorder (MDD), commonly referred to as depression, is one of the most prevalent mental health conditions among veterans. It goes far beyond occasional sadness — depression is a persistent condition that affects how you think, feel, and handle daily activities. For veterans, depression often develops during or after military service due to combat exposure, traumatic experiences, loss of fellow service members, difficulty transitioning to civilian life, or chronic pain from service-connected injuries.
Depression manifests through a range of symptoms including persistent low mood, loss of interest in activities you once enjoyed, fatigue, difficulty concentrating, changes in appetite and sleep patterns, feelings of worthlessness or excessive guilt, and in severe cases, recurrent thoughts of death or suicide. These symptoms can make it difficult to maintain employment, sustain personal relationships, and carry out even basic daily tasks.
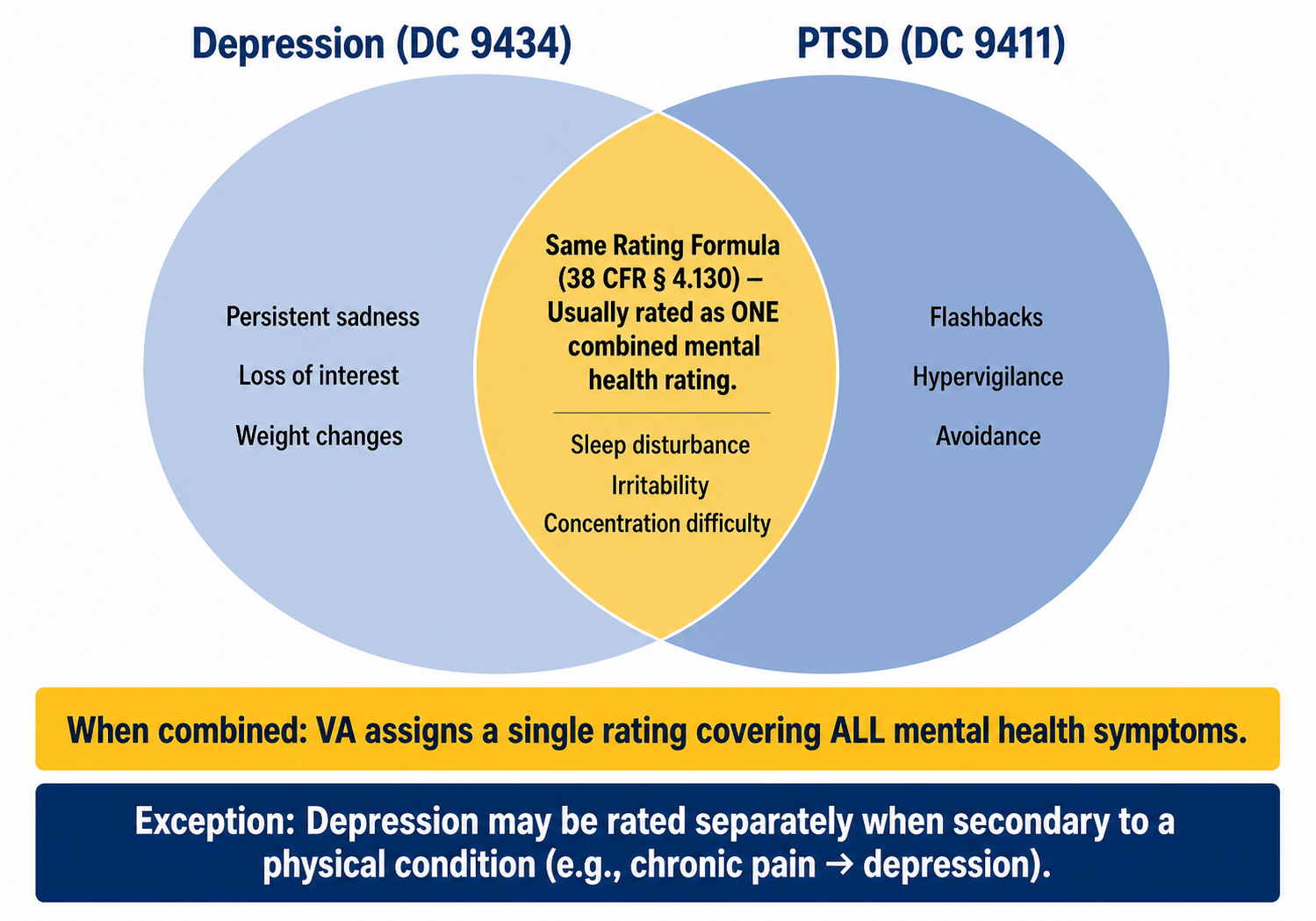
The VA rates depression under the same General Rating Formula for Mental Disorders used for PTSD, anxiety, and other mental health conditions. This means the VA evaluates the overall impact of your depressive symptoms on your occupational and social functioning. If you are already rated for another mental health condition like PTSD, your depressive symptoms are typically evaluated together under one combined rating rather than receiving a separate rating for each diagnosis.
VA diagnostic code for depression
Depression is rated under Diagnostic Code (DC) 9434 per 38 CFR § 4.130, Schedule of Ratings — Mental Disorders. DC 9434 specifically covers Major Depressive Disorder, which is the clinical diagnosis most commonly associated with what veterans experience as chronic depression.
All mental health conditions rated under 38 CFR § 4.130 use the same General Rating Formula. This means the rating criteria for depression are identical to those for PTSD, anxiety, bipolar disorder, and other mental health conditions in this section. The VA evaluates the overall impact of your mental health symptoms on occupational and social functioning, regardless of the specific diagnosis.
Rating criteria for depression
The VA assigns depression ratings at six possible levels. Here’s what each rating requires and what it pays in 2026:
0% rating
Criteria: A mental condition has been formally diagnosed, but symptoms are not severe enough to interfere with occupational and social functioning or to require continuous medication.
Monthly payment: $0 (but establishes service connection, which matters for future increases and secondary claims)
10% rating — $180.42/month
Criteria: Occupational and social impairment due to mild or transient symptoms which decrease work efficiency and ability to perform occupational tasks only during periods of significant stress, or symptoms controlled by continuous medication.
What this looks like: You generally function well at work and in relationships, but stressful periods bring noticeable depressive episodes. You may take antidepressants that effectively manage your symptoms most of the time, but you still have occasional low periods during high-stress situations.
30% rating — $552.47/month
Criteria: Occupational and social impairment with occasional decrease in work efficiency and intermittent periods of inability to perform occupational tasks (although generally functioning satisfactorily, with routine behavior, self-care, and conversation normal), due to such symptoms as:
- Depressed mood
- Anxiety
- Suspiciousness
- Panic attacks (weekly or less often)
- Chronic sleep impairment
- Mild memory loss (such as forgetting names, directions, recent events)
What this looks like: You hold a job but have stretches where depression clearly drags down your productivity. You may call in sick more often during depressive episodes, withdraw from coworkers, or struggle to stay focused. Sleep is frequently disrupted, and you find yourself forgetting things more than usual.
50% rating — $1,132.90/month
Criteria: Occupational and social impairment with reduced reliability and productivity due to such symptoms as:
- Flattened affect
- Circumstantial, circumlocutory, or stereotyped speech
- Panic attacks more than once a week
- Difficulty in understanding complex commands
- Impairment of short- and long-term memory (e.g., retention of only highly learned material, forgetting to complete tasks)
- Impaired judgment
- Impaired abstract thinking
- Disturbances of motivation and mood
- Difficulty in establishing and maintaining effective work and social relationships
What this looks like: Depression regularly and noticeably affects your work performance and personal life. You may struggle to complete tasks on time, have difficulty maintaining friendships, and find that your motivation is consistently low. Coworkers and family members have likely noticed changes in your behavior and reliability.
70% rating — $1,808.45/month
Criteria: Occupational and social impairment, with deficiencies in most areas, such as work, school, family relations, judgment, thinking, or mood, due to such symptoms as:
- Suicidal ideation
- Obsessional rituals which interfere with routine activities
- Speech intermittently illogical, obscure, or irrelevant
- Near-continuous panic or depression affecting the ability to function independently, appropriately, and effectively
- Impaired impulse control (such as unprovoked irritability with periods of violence)
- Spatial disorientation
- Neglect of personal appearance and hygiene
- Difficulty in adapting to stressful circumstances (including work or a work-like setting)
- Inability to establish and maintain effective relationships
What this looks like: Depression dominates most areas of your life. You may have difficulty holding a job because you cannot consistently get out of bed, concentrate, or interact with coworkers. Relationships are severely strained or nonexistent. You may have thoughts of suicide, neglect personal hygiene, and find that even simple tasks feel overwhelming.
100% rating — $3,938.58/month
Criteria: Total occupational and social impairment, due to such symptoms as:
- Gross impairment in thought processes or communication
- Persistent delusions or hallucinations
- Grossly inappropriate behavior
- Persistent danger of hurting self or others
- Intermittent inability to perform activities of daily living (including maintenance of minimal personal hygiene)
- Disorientation to time or place
- Memory loss for names of close relatives, own occupation, or own name
What this looks like: You cannot work in any capacity and cannot maintain meaningful social relationships. Your depression is so severe that you may require assistance with basic daily tasks like bathing, eating, or managing finances. Hospitalization for suicidal behavior may have occurred.
What evidence do you need?
Building a strong depression claim requires several types of evidence:
Service records
- Service treatment records showing any in-service mental health complaints, diagnosis, or treatment
- Personnel records that may show behavioral changes — declining performance evaluations, disciplinary actions, or early separation that could indicate onset of depression
- Deployment records, combat exposure, or documentation of stressful duty assignments
Medical evidence
- Current diagnosis of Major Depressive Disorder from a qualified mental health professional (psychiatrist, psychologist, or licensed clinical social worker)
- Treatment records showing ongoing symptoms and their severity over time
- Medication records, including any antidepressant prescriptions and dosage changes
- Hospitalization records if applicable, especially for suicidal ideation or attempts
Nexus letter
A medical opinion letter connecting your depression to your military service. This is critical if your depression was not diagnosed during service. A strong nexus letter states that your depression is “at least as likely as not” related to your military service and explains the medical reasoning. If claiming depression as secondary to another condition (such as chronic pain or TBI), the nexus letter should explain how that primary condition caused or aggravated your depression.
Buddy statements
Statements from fellow service members, family, or friends who can describe:
- Changes in your mood and behavior during or after service
- How your depression affects your daily life, work, and relationships
- Specific examples of depressive episodes they’ve witnessed
- Comparisons of your behavior before and after military service
Personal statement
Your own detailed account of how depression affects your daily life, work, and relationships. Be specific and describe your worst days — not your best. For example, instead of “I feel sad a lot,” write “There are 2-3 days per week where I cannot get out of bed before noon, which has caused me to lose two jobs in the past year. I haven’t seen friends in six months because I can’t bring myself to leave the house.”
C&P exam tips for depression
The Compensation & Pension (C&P) exam is often the most important part of your depression claim. Here’s how to prepare:
What the examiner evaluates
The examiner uses the DSM-5 criteria for Major Depressive Disorder and assesses your symptoms against the VA’s rating criteria. They evaluate:
- Frequency and severity of depressive episodes
- Impact on occupational functioning (can you work reliably?)
- Impact on social functioning (relationships, social activities, isolation)
- Whether you need continuous medication
- Suicidal ideation or attempts
- Your overall level of impairment in daily functioning
How to prepare
- Don’t minimize your symptoms. Veterans often say “I’m fine” or “I’m dealing with it” out of habit. Describe your worst days honestly, not your best days.
- Be specific with examples. Instead of “I have low motivation,” say “I went three weeks without showering last month and my wife had to intervene. I’ve stopped cooking and only eat when someone puts food in front of me.”
- Bring a family member or close friend. They can provide perspective on symptoms you may not recognize in yourself, such as how much you’ve withdrawn or how your mood has changed.
- Mention all symptoms. Discuss sleep disruption, appetite changes, concentration problems, fatigue, feelings of worthlessness, loss of interest, irritability, and suicidal thoughts if applicable.
- Don’t skip the exam. A missed C&P exam will result in your claim being denied.
Common mistakes
- Telling the examiner “I’m managing” or “things are okay” — this signals lower severity
- Not disclosing suicidal thoughts if you have them (this is critical for 70%+ ratings)
- Presenting a cleaned-up version of yourself rather than reflecting your typical daily state
- Being inconsistent with what’s documented in your medical records
Common secondary conditions linked to depression
Depression frequently causes or aggravates other conditions. These can be claimed as secondary service-connected disabilities:
- Sleep apnea — Depression-related weight gain (often worsened by antidepressant side effects and reduced physical activity) is a significant risk factor for developing obstructive sleep apnea.
- GERD — Chronic stress and anxiety associated with depression can increase stomach acid production and worsen gastrointestinal symptoms. Antidepressant medications can also contribute to GERD.
- Migraines — Depression and migraines share common neurological pathways. Veterans with depression are significantly more likely to experience chronic headaches and migraines.
- Erectile dysfunction — SSRI antidepressants are well-documented to cause sexual dysfunction, and the psychological effects of depression also reduce libido and sexual performance.
How to calculate your monthly payment
Your total VA disability payment depends on your combined rating across all service-connected conditions, not just depression alone. Use our VA disability calculator to:
- Calculate your combined rating with multiple conditions
- See how VA math combines ratings differently than simple addition
- Estimate your monthly payment including dependents
For the full breakdown of payment amounts at every rating level, see our 2026 VA disability pay rates page.
Disclaimer: This content is for informational purposes only and does not constitute legal or medical advice. For personalized guidance on your VA disability claim, consult a VA-accredited Veterans Service Organization (VSO), attorney, or claims agent. You can find accredited representatives at VA.gov.
Frequently Asked Questions
What is the most common VA rating for depression?
The most commonly assigned rating for depression is 30% or 50%. However, ratings range from 0% to 100% depending on the severity of symptoms and their impact on your occupational and social functioning. Many veterans with moderate depression that affects work performance receive a 50% rating.
Can you get 100% VA disability for depression alone?
Yes. A 100% schedular rating for depression requires total occupational and social impairment. This means symptoms so severe that you cannot maintain employment or meaningful social relationships — for example, persistent suicidal behavior, inability to perform basic activities of daily living, or complete social withdrawal.
Can depression be rated separately from PTSD?
Generally, no. The VA's rule against pyramiding (38 CFR § 4.14) prevents separate ratings for conditions with overlapping symptoms. Since depression and PTSD are both rated under the General Rating Formula for Mental Disorders, the VA typically assigns a single rating that accounts for all mental health symptoms. However, if depression is diagnosed as a distinct condition secondary to a physical service-connected disability, a separate rating may be possible.
How do I prove my depression is service-connected?
You need three things: a current diagnosis of depression from a qualified mental health professional, evidence of an in-service event or stressor, and a medical nexus opinion linking your depression to service. Depression can also be claimed as secondary to another service-connected condition like chronic pain, PTSD, or TBI.
Does medication for depression affect my VA rating?
Yes. If your depression requires continuous medication to manage symptoms, you meet at least the 10% rating criteria. Additionally, side effects from antidepressants (such as sexual dysfunction or weight gain) may qualify as secondary conditions with their own separate ratings.
Sources
Every rating percentage, diagnostic code, and dollar figure on this page is sourced from the references below. See our editorial policy for how we choose and verify sources.
- 38 CFR § 4.130 — Schedule for Rating Disabilities — eCFR
- VA Disability Compensation — U.S. Department of Veterans Affairs
- VA Disability Compensation Rates — U.S. Department of Veterans Affairs
- Diagnostic Code 9434 — VA Schedule for Rating Disabilities — eCFR
Related Guides
Related Conditions
Popular VA Rating Guides
- PTSD VA Rating: 10%, 30%, 50%, 70%, 100% (DC 9411, 2026 Guide)
- Sleep Apnea VA Rating 2026: 0%, 30%, 50%, 100% (CPAP Rule Update)
- Sciatica VA Rating: 10%, 20%, 40%, 60% & 80% Guide (2026)
- Tinnitus VA Disability Rating
- Hearing Loss VA Rating: 0%–100% Audiometric Chart (DC 6100, 2026)
- Back Pain VA Rating: 10%, 20%, 40%, 50%, 100% (DC 5237, 2026)
- Knee Pain VA Disability Rating
- Migraines VA Disability Rating
This content is for informational purposes only and does not constitute legal or medical advice. For personalized guidance, consult a VA-accredited VSO, attorney, or claims agent.
