The Compensation and Pension (C&P) exam is the single most consequential step in a VA disability claim. The examiner’s report drives the rating decision more than service treatment records, more than buddy statements, more than personal statements. What you say in 30 to 90 minutes decides what the VA pays you for the rest of your life.
Most veterans do not lose claims because they lied. Most lose claims, or lose levels of rating, because they minimize. They downplay. They put on the same “I’m fine, thanks” face they put on for a doctor’s appointment, a job interview, or a family dinner — and the examiner writes down exactly that.
This guide covers the specific phrases that hurt claims, the ones that help, and how to think about the exam differently than a normal medical visit.
The frame: this is not a normal doctor’s appointment
When you see your primary care provider, the goal is to feel better. You report what’s wrong, they treat it, you describe progress at the next visit. The social script rewards understatement: “It’s a little better.” “I’m getting by.” “I had a rough week but I’m okay.”
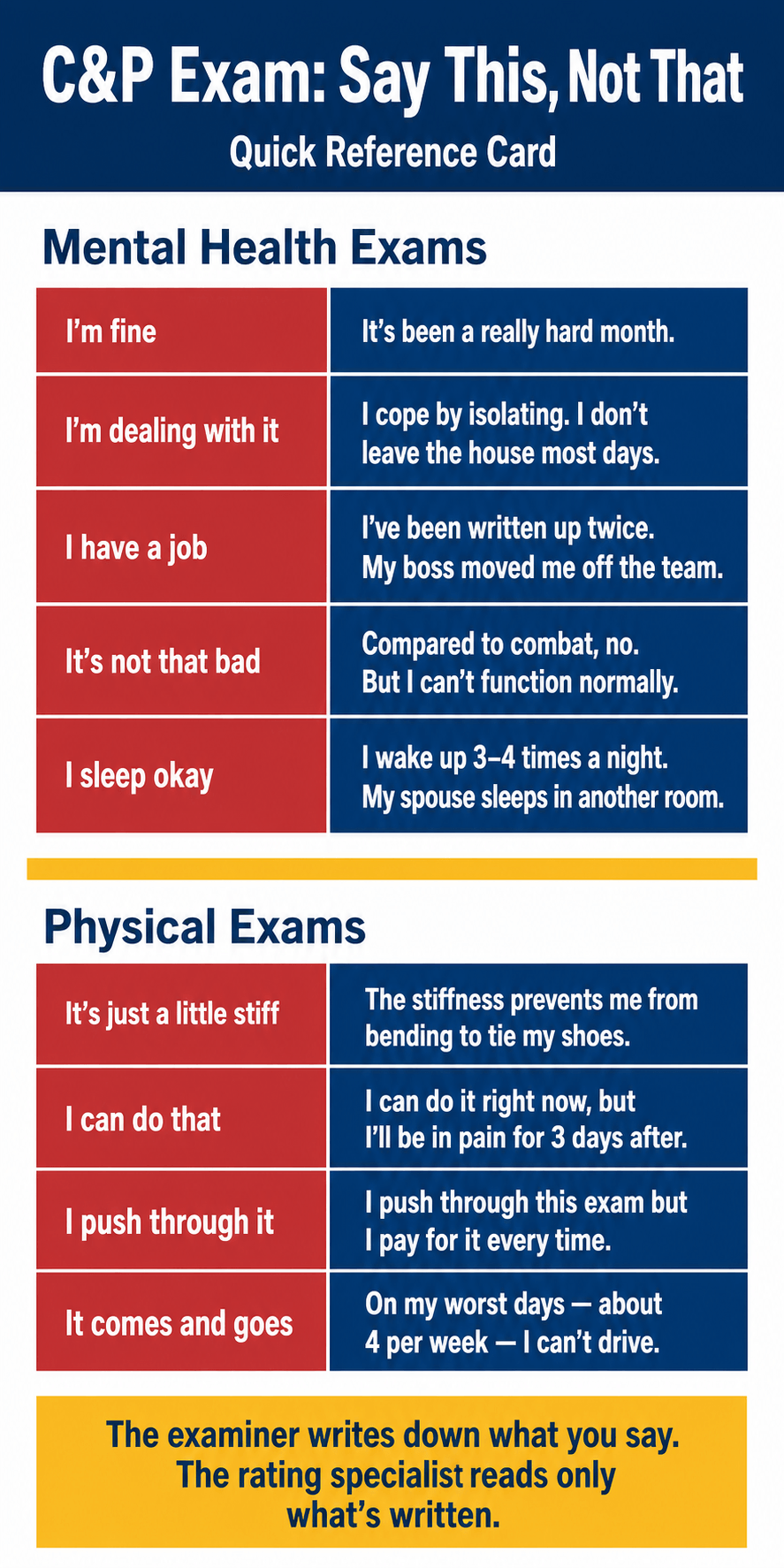
The C&P exam runs on the opposite logic. The examiner is producing an evaluation, not delivering care. The rating specialist who reads the report has never met you and never will. The only window they have into your condition is what the examiner wrote down — and what the examiner wrote down is built almost entirely from what you said in the exam room.
If you describe a “decent week,” that is what the examiner records. If you describe your average week — say, the four days last month you couldn’t get out of bed — that is what gets recorded. Same person, same condition, dramatically different rating decisions.
Honesty matters. Exaggeration backfires (more on that below). But honest about the actual range of how the condition affects you, including the worst end of that range, is the standard the rating system was designed for.
What not to say at a PTSD or mental health C&P exam
These are the phrases that most often cost veterans rating levels on PTSD, depression, anxiety, MDD, and related claims rated under 38 CFR § 4.130:
“I’m fine.”
Said reflexively to the question “How are you doing?” This single phrase, recorded in the exam report, can tank a claim. The rating criteria measure occupational and social impairment; “I’m fine” is the textbook description of no impairment. If you walk in and say this without elaboration, you have just told the examiner you do not need a rating.
What to say instead: “It’s been a hard month — I can describe what’s been going on if that helps."
"I have good days and bad days.”
True for almost every veteran with PTSD or depression. The problem is when this phrase is left vague. The examiner has nothing concrete to write. The rating decision defaults to a lower tier because there is no documented severity.
What to say instead: “On a bad week — which is most weeks — I can’t sleep more than three hours, I avoid leaving the house, I lose my temper with my family, and I have intrusive thoughts I can’t control. On a good day I can run errands. I have maybe four good days a month."
"I have a job.”
Said as a complete sentence with no follow-up. The 50%, 70%, and 100% PTSD criteria all turn on occupational impairment. If your only statement about work is “I have a job,” the examiner has no evidence of impairment to record.
What to say instead: “I have a job. I miss two to four days a month due to symptoms. I’ve changed jobs three times in the last five years because I couldn’t get along with supervisors. My current employer is my brother-in-law, which is the only reason I haven’t been fired for absences."
"I’m not suicidal.”
Veterans say this defensively, often because they think disclosure could lead to involuntary commitment or affect firearms ownership. But suicidal ideation — even passive ideation, even fleeting thoughts — is one of the symptoms that distinguishes a 70% rating from a 50% rating. Denying it when it is present means the examiner cannot record what is medically true.
If you have suicidal thoughts, including passive thoughts (“I wouldn’t mind if I didn’t wake up”), say so. Active intent or a plan would prompt a separate clinical response, but the typical passive ideation seen in PTSD and depression is recorded as a symptom — not as a reason for hospitalization.
”I’m dealing with it.”
Means nothing on a rating. Same problem as “I’m fine.”
What to say instead: “I cope. The cost of coping is that I’m exhausted, I drink more than I should, I’ve lost my temper with my kids three times this month, and I haven’t seen friends since 2022."
"It’s gotten better since I started medication.”
True for many veterans, but the rating criteria for the 10% level explicitly include “symptoms controlled by continuous medication.” If the medication is what’s keeping you functional, that is what the examiner needs to know — including the side effects.
What to say instead: “Sertraline brings me from a 9 to a 6, but it gives me sexual side effects, weight gain, and emotional flatness. Without it I cannot function at all. I’ve been on continuous medication for [X] years.”
What not to say at a physical condition C&P exam
For musculoskeletal conditions (back, knee, shoulder, neck), the rating math is mostly mechanical: range of motion measurements drive the rating, with adjustments for pain on motion, flare-ups, and functional loss under DeLuca v. Brown.
”I can do that.”
Said when the examiner asks if you can perform a particular movement. Often the veteran can do the movement once, in the exam, on their best day, with the examiner watching. That is exactly the wrong measurement. The rating is supposed to capture functional loss across normal life, including flare-ups.
What to say instead: “I can do it once like this. If I do it ten times in a row, by the fifth or sixth my back locks up. After yard work I can’t get out of bed for two days."
"It’s just a little stiff.”
Same minimization problem. “Stiffness” implies mild limitation; the rating tiers turn on degrees of forward flexion. Either give the actual ranges, or describe the functional consequences.
What to say instead: “I can’t bend forward to tie my shoes. I sit on a chair to put them on. I can’t lift my four-year-old without flaring up."
"I take Advil for it.”
Said as if it explains the situation. It does not. Many veterans take ibuprofen daily for severe service-connected pain, but the examiner records “OTC NSAID” and the rating specialist reads that as a mild condition.
What to say instead: “I take 800mg ibuprofen three times a day, plus a muscle relaxer at night, plus tramadol prescribed by my VA primary care for breakthrough pain. The ibuprofen has caused stomach issues that I’m now seeing GI for."
"I push through it.”
Veterans take pride in this. The rating system penalizes it. If you push through symptoms to do the exam, the examiner records the better-than-actual function, not the cost. Mention the cost.
What to say instead: “I’m pushing through this exam. I’ll pay for it tomorrow — I won’t be able to walk for two days after the range-of-motion testing. That’s normal for me when I exceed my baseline.”
On exaggeration: don’t
Exaggeration is the other failure mode, and examiners are trained to detect it. Most mental health C&P examiners use validity measures (M-FAST, MMPI-2-RF, structured interviews) that flag inconsistent presentations. A claim flagged as “symptom magnification” or “invalid presentation” is functionally dead — the rating specialist reads it as evidence to discount everything else in the file.
The bar is honest, complete, and grounded in the worst end of your normal range. Not the best end. Not above the actual range.
If you are not sure where the line is: describe the symptoms you actually have, in the actual frequency they actually occur, with the actual impact they actually have. That is the line.
What to bring
A short, written list, in your own handwriting, of:
- The five worst symptoms of the condition.
- How often each occurs (daily, weekly, monthly).
- What each symptom prevents you from doing.
- All medications, side effects, and other treatments you’ve tried.
- The frequency and severity of flare-ups, including the most recent one.
You can refer to it during the exam. Bring buddy statements from a spouse or close family member describing what they observe — examiners give those significant weight when paired with consistent self-report.
For more on exam preparation, see our condition-specific C&P exam checklists and how to file a VA disability claim.
After the exam
Request a copy of your DBQ through VA.gov as soon as it’s available. Read it carefully. If the examiner missed something important — frequency of flare-ups, medication side effects, suicidal ideation that you reported — file a written statement correcting the record. The rating specialist will see it.
If the rating decision is lower than the evidence supports, you have three appeal lanes: a Higher-Level Review, a Supplemental Claim with new evidence, or a Board Appeal. The C&P exam is consequential, but it is not the last word.
Frequently Asked Questions
What should you not say at a PTSD C&P exam?
Do not minimize symptoms with phrases like 'I'm fine,' 'it's not that bad,' or 'I have good days.' Do not say you have a job that's going well unless that's accurate, since the rating criteria for PTSD center on occupational and social impairment. Do not deny suicidal thoughts if you have them — examiners need an accurate clinical picture, not a guarded one. Describe your worst weeks, not your best day.
Can what I say at the C&P exam lower my rating?
Yes. The examiner is producing an evaluation that the rating specialist relies on. If you minimize symptoms, deny medication side effects, or describe a level of function higher than your actual baseline, the resulting Disability Benefits Questionnaire (DBQ) will reflect that — and your rating decision will be based on it. The examiner is not your doctor. They do not know you. Their report is what counts.
Should I exaggerate symptoms at my C&P exam?
No. Exaggeration backfires. Examiners are trained to identify inconsistent presentations, and most use validity measures during mental health evaluations. An exam where reported symptoms exceed observed function is often labeled 'symptom magnification' or 'invalid' in the report, which the rating specialist reads as evidence to discount your claim. The right standard is honest, complete, and grounded in your worst days — not your best, not exaggerated.
Can I refuse to answer a question at a C&P exam?
You can decline to answer, but doing so often hurts the claim. The examiner needs the information to support a higher rating. If a question makes you uncomfortable, you can say so — 'this is hard to talk about' is a legitimate response, and the examiner should note it. Refusing categorically is different from being honest about how difficult disclosure is.
Should I bring notes to my C&P exam?
Yes. Bring written notes describing the worst version of your condition, frequency and triggers of flare-ups, medication side effects, and the specific ways the condition limits work, sleep, relationships, and daily activities. You can refer to them during the exam. Memory often fails under the stress of the appointment, and notes prevent omissions that would otherwise cost you on the rating decision.
Sources
Every rating percentage, diagnostic code, and dollar figure on this page is sourced from the references below. See our editorial policy for how we choose and verify sources.
- VA Disability Benefits Questionnaires (DBQs) — U.S. Department of Veterans Affairs
- 38 CFR § 4.130 — Schedule of ratings—Mental disorders — eCFR
- M21-1 Adjudication Procedures Manual — U.S. Department of Veterans Affairs
Related Guides
This content is for informational purposes only and does not constitute legal or medical advice. For personalized guidance, consult a VA-accredited VSO, attorney, or claims agent.

